Tendon pain is common after 50, particularly in active women, but it is rarely something you just have to “live with”. Ageing, hormone changes and lifestyle all influence tendon health, yet the biggest factor is often how we load and use our bodies. A structured plan combining targeted exercise rehabilitation and, where appropriate, modern treatments such as shockwave therapy can help many people reduce pain, restore strength and keep doing the activities they enjoy.
At Thorpes Physiotherapy, we help people understand why their tendon pain has started, what it means, and how to move forward with confidence.
Why tendon pain becomes more common after 50
Tendons connect muscle to bone and act like strong cables that help you move, absorb force and stay stable.
As we move through our 40s, 50s and beyond, several changes can make tendons more vulnerable:
- Collagen (the protein that gives tendons their strength) is replaced more slowly
- Tendons may become slightly stiffer and less able to cope with sudden changes in load
- Muscle strength and mass tend to reduce if we are not doing enough resistance exercise
For women, changes in oestrogen around the menopause can also influence tendon health. Some research suggests these hormonal shifts may affect how tendons repair themselves and cope with load.
Importantly, tendon pain is usually not about “wearing out” in a simple way. More often, it is about a mismatch between what the tendon is asked to do and what it is currently strong enough to handle.
Common areas affected after 50 include:
- Shoulder (rotator cuff)
- Elbow (tennis or golfer’s elbow)
- Hip (gluteal tendons at the side of the hip)
- Knee (patellar tendon)
- Achilles tendon and plantar fascia (heel and foot)
How tendon pain impacts daily life and activity
Tendon pain is often most noticeable with movement and load. Many people find it:
- Achy or sharp when walking, climbing stairs or going uphill
- Sore first thing in the morning or after sitting for a while
- Worse during or after activities like tennis, running, gardening or gym classes
Over time, tendon pain can start to chip away at confidence. You might avoid certain movements, stop your usual exercise class, or feel anxious about making things worse. This loss of activity can then weaken the tendon and surrounding muscles further, creating a frustrating cycle.
Sleep can also be affected. For example, people with hip or shoulder tendon pain often struggle to lie on the sore side. Poor sleep then reduces energy and motivation to exercise, again making recovery harder.
Common myths about ageing and pain
Many people over 50 have been told unhelpful or outdated messages about pain. Here are some myths we regularly hear in clinic:
- “It is just your age, nothing can be done.”
- Age is one factor, but it is rarely the full story.
- Tendons can adapt and get stronger at any age with the right stimulus.
- “If you have tendon pain, you must rest completely.”
- Short-term rest can settle a flare-up, but complete long-term rest often leads to more stiffness, weakness and pain when you try to return to activity.
- “Pain equals damage.”
- Scans have shown that many people with tendon changes on imaging do not have pain, and some with pain have relatively mild changes.
- Pain is influenced by sensitivity, load, sleep, stress and many other factors.
- “I have arthritis, so tendon pain is inevitable.”
- Arthritis and tendon problems can exist together, but they are not the same thing.
- Strengthening and load management can still make a real difference, even when arthritis is present.
Challenging these myths is often the first step in regaining control.
What most people get wrong about treating tendon pain
When tendon pain appears, many people understandably reach for quick fixes. Common but unhelpful approaches include:
- Only resting and hoping it will disappear
- Repeatedly stretching a painful tendon in every direction
- Relying solely on massage or short-term pain relief
- Jumping straight back to full activity as soon as it feels a little better
These strategies may offer brief relief but rarely change how strong and tolerant the tendon is. Without addressing strength and load, pain often returns when you increase your activity again.
Another common issue is stopping treatment too early. Tendons adapt slowly. They often need weeks to months of gradual loading and progression to build lasting resilience.
The power of movement: why rest is not always best
Movement is one of the most powerful tools we have for tendon health. Rather than complete rest, most painful tendons respond better to relative rest and graded loading.
Relative rest means:
- Reducing or temporarily changing the activities that really flare your pain
- Keeping up with gentler activities that your body tolerates well
- Avoiding long periods of total inactivity where possible
Graded loading means:
- Starting with manageable exercises that challenge the tendon and muscles just enough
- Slowly increasing the difficulty or weight over time
- Allowing enough recovery between sessions so the tendon can adapt
Research has shown that well-designed exercise programmes can improve pain and function in many common tendinopathies. While not every tendon problem behaves the same, movement-based approaches usually form the foundation of effective care.
How exercise rehab can restore strength and mobility
Targeted exercise rehabilitation is different from simply “doing more exercise”. It is a structured programme designed around your specific tendon, your current ability and your goals.
A physiotherapy-led tendon rehab plan often includes:
- Strength exercises to build the muscle groups supporting the tendon
- Slow, controlled loading (for example, slowly lowering the heel off a step for Achilles problems)
- Progression over time, using weights, resistance bands or body weight
- Functional movements that relate to your everyday activities or sports
For someone over 50, especially women, we also consider:
- Bone health and balance
- Previous injury history
- Menopausal status and general fitness
At Thorpes Physiotherapy, we first carry out a thorough assessment to understand:
- Which tendon is irritated
- Which movements or loads provoke your pain
- How strong and coordinated the surrounding muscles are
From there, we build a staged plan. Early exercises might be simple, such as isometric (static) holds to reduce pain. Later stages may involve more challenging strength and functional drills that prepare you for walking, running, tennis, gardening or gym work.
For more about how we assess and manage tendon issues, you can read our tendon information page: https://thorpesphysiotherapy.com/tendon-problems/.
How shockwave therapy supports tendon recovery
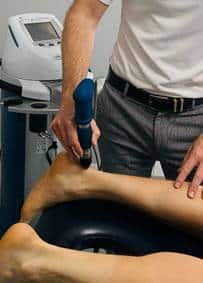
Alongside exercise rehabilitation, modern treatments such as shockwave therapy can be helpful for some tendon problems.
What is shockwave therapy?
Extracorporeal shockwave therapy (often shortened to “shockwave”) uses high-energy sound waves delivered through a hand-held device applied to the skin over the painful area. These waves are thought to:
- Stimulate local blood flow
- Promote tissue remodelling
- Influence pain signalling
Shockwave is usually used for longstanding tendon issues where pain has persisted for several months despite rest or basic self-management. Conditions where evidence and clinical experience suggest benefit include:
- Plantar fasciitis (heel and foot pain)
- Achilles tendinopathy
- Some cases of tennis elbow
- Some forms of hip and shoulder tendinopathy
It is important to remember that responses vary. Shockwave is not a guaranteed cure, but for some people it provides a valuable boost alongside a good rehab programme.
What does shockwave treatment feel like?
Most people describe shockwave therapy as uncomfortable but tolerable. During a session, the therapist places the device on the skin with some gel and gradually adjusts the settings to find a level you can manage.
A typical session lasts around 10 to 20 minutes, depending on the area being treated. You can usually walk out of the clinic and carry on with your day afterwards. Some soreness for a day or two is common.
Why shockwave and exercise work well together
Shockwave therapy is often most effective when combined with a targeted exercise programme.
The shockwave may help to:
- Reduce pain to a more manageable level
- Stimulate a healing response in the tendon area
Exercise rehab then:
- Builds strength and resilience
- Teaches the tendon to cope with the loads of your day-to-day life and hobbies
At Thorpes Physiotherapy, we do not rely on technology alone. We combine modern treatments like shockwave with clear education, movement coaching and progressive strengthening.
What to expect at Thorpes Physiotherapy
When you visit Thorpes Physiotherapy for tendon pain, the focus is on clarity and a clear plan.
Your physiotherapist will typically:
- Listen to your story – how and when your pain started, and how it affects your life
- Examine your movement, strength and tendon irritability
- Discuss any relevant medical history, including menopause, arthritis or previous injuries
- Explain in plain language what is likely going on and why your tendon is sensitive
From there, you will work together on a plan that may include:
- A tailored exercise rehabilitation programme
- Advice on how to adjust your activities in the short term without stopping everything you enjoy
- Hands-on treatment if appropriate
- Discussion of whether shockwave therapy is likely to help in your particular case
If shockwave is suitable, we will explain:
- How many sessions are typically recommended
- What you can reasonably expect to feel during and after treatment
- How it will fit alongside your exercise plan
Our aim is always to help you feel informed, supported and confident about the next steps.
Taking action: your next steps if you have tendon pain
If you are living with tendon pain, consider the following:
- If pain has been present for more than a few weeks and is affecting your activity or sleep, it is sensible to seek a professional assessment
- If you are avoiding movement for fear of making things worse, guided rehab can give you a safer way forward
- If you have tried rest and simple stretches without lasting improvement, more structured loading and possible adjuncts like shockwave may be worth exploring
You do not have to have everything “bad enough for surgery” before asking for help. Often, the earlier you get a clear plan, the more options you have.
If you would like to explore whether our approach is right for you, you can book a free Discovery Visit at Thorpes Physiotherapy. This is a chance to talk through your symptoms, ask questions, and understand your options without pressure.
Book free DV:
- Online: Book free DV
- Phone: 01276 37670
At Thorpes Physiotherapy, we are always happy to discuss whether physiotherapy, exercise rehabilitation and treatments like shockwave therapy could be appropriate as part of your wider care.
If you feel ready to book an initial consultation, where we will diagnose your problem and make a start on treatment, then you can book online through clicking the button below

If you are unsure if Physiotherapy or podiatry is the correct route for you and would like to speak to one of our experts first, free of charge, then please click here.
Warm regards

Jonathan Smith (MSc BSc FSOMM MCSP SRP)
Director of Thorpes Physiotherapy
